 “Flat feet” is a term we often discuss here at The Kilmore and Wallan Podiatry Clinic. Often people will present with concerns about having, or loved ones having the dreaded “flat feet”.
“Flat feet” is a term we often discuss here at The Kilmore and Wallan Podiatry Clinic. Often people will present with concerns about having, or loved ones having the dreaded “flat feet”.
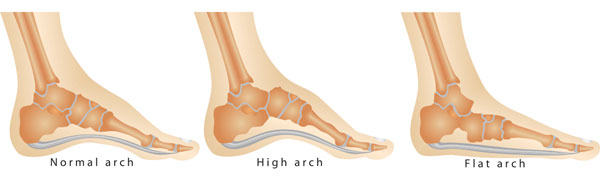
Flat feet are typically feet that little to no visible or feet that roll in excessively. Flat feet were once thought of as being a disaster comparable to the black plague, but now we know that there isn’t really one perfect or ideal foot posture that we all need to strive towards. We are all somewhere on the spectrum, from flat feet (pes planus) to high arch (pes cavus). When it comes to preventing and managing injuries, it is our movement patterns rather than posture that we focus on.
Over-pronation, or flat feet, is a common biomechanical problem that occurs when a person’s arch collapses too far upon weight bearing, and is said to be “over-pronated”.
Pronation is the natural motion of the foot as it roles inward and flattens out when the foot makes contact with the ground. Pronation is part of the body’s natural complex shock absorption and allows the foot to adapt to the contour of the ground. Too much pronation will cause the arch of the foot to flatten excessively placing stress and pressure on the tissues and ligaments of the foot.
The best way to determine if you over pronate is to visit a Podiatrist who can do a full gait analysis on a treadmill or on the ground. It is not only the amount of over pronation which is important but the timing of it during the gait cycle as well that needs to be assessed.
This is quite a common problem and may lead to a number of injuries, especially in runners, including:
- Arch Pain
- Shin splints
- Plantar fasciitis
- Heel Pain
- Achilles tendon problems
- Stiff big toe (Hallux limitus)
- Heel spurs
- Bunions (Hallux valgus)
- Knee pain
- Lower back pain
- Pain in the ball of the foot (metatarsalgia or Morton’s neuroma)
Treatment and Prevention
Below are some of the treatment protocols that may be used:
- Orthotics provide the required support to effectively reduce excessive pronation and guide the foot to move in its most efficient way. Orthotics should be designed specifically for the patient’s feet to address the unique needs of the patient.
- Footwear should also be examined to ensure there is a proper fit. Footwear with a firm heel counter is often recommended for extra adequate control, support and stability. Improperly fitting footwear can lead to additional foot problems.
- Strapping/Taping – Taping the foot in a certain way provides support for the foot as well as stability and may be used in acute cases or as a first line treatment.
- Exercises – These are used to strengthen certain muscles in order to achieve better foot function.
- Stretching protocols – This help in loosening tight muscles and ligaments to prevent further strain.
- Joint manual mobilisation – This helps joints that may have become stiff or fixed to loosen up and in turn allowing for better foot function.
